Have you heard that Orange Coast Women’s Medical Group has partnered with Hoag Breast Centers to provide a comprehensive and multidisciplinary approach to breast care? It’s true! This partnership brings together specialized board certified radiologists, pathologist, breast surgeons, radiation and medical oncologists who consult directly with your OCWMG Provider to determine the best course of treatment for each individual patient.
Mammography Facts

DID YOU KNOW…
- Mammography has reduced breast cancer mortality rates by 1/3 in the United States since 1990
- 1 in 6 breast cancers occur in women between the ages of 40 and 49
- 3/4 of women diagnosed with breast cancer have no family history and are not considered “high risk”
Mammography is an important step in taking care of yourself and your breast. A mammogram is an x-ray of the breast that is used to find breast changes. This specific type of breast exam is used to aid in the early detection and diagnosis of breast diseases in women. This quick medical exam uses noninvasive X-ray targeted to each breast, producing pictures that a Breast Specialized Radiologist can use to identify and treat any abnormal areas, possibly indicating the presence of cancer
Why is everyone talking about Mammograms?
Annual mammograms can detect the most common types of breast cancer at it’s earliest stage when it is most treatable. In fact, mammograms show changes in the breast up to two years before a patient or physician can feel them. Mammograms can also prevent the need for extensive treatment for advanced cancers and improve chances of breast conservation. Current guidelines from the American College of Radiology, the American Cancer Society, and the Society for Breast Imaging recommend that women receive annual mammograms starting at age 40 – even if they have no symptoms or family history of breast cancer.
We perform your mammogram, but do you know who reads your mammogram?
Dr January Lopez, that’s who! Dr Lopez is the Director of Hoag Breast Center, she and her elite team of experts in breast imaging interpret, diagnose and assist in navigating your breast health in collaboration with your OCWMG provider. Dr Lopez and her team also perform diagnostic procedures, including breast ultrasound, breast biopsies, wire localizations and sentinel node mapping. They are dedicated to providing the highest level of quality imaging services to all patients and healthcare providers.
-
Why Hoag Breast Program?
- Hoag is the first and only breast center in Orange County designated as a Certified Quality Breast Center of Excellence by the National Consortium of Breast Centers.
- Hoag has the largest team of radiologists dedicated to breast imaging in Orange County and are committed to providing the highest level of quality, care, and compassion for women undergoing screening, diagnosis, treatment and follow-up for breast cancer.
- Hoag’s dedicated radiologists surpass national quality benchmarks for mammography year after year. Why does this matter? It means that if you have breast cancer, Hoag’s radiologists are more likely to detect it on your mammogram than the average radiologist.
- Hoag’s dedicated breast radiologists are less likely to require additional imaging after your screening exam in order to reassure a normal result.

Screening Guidelines for Breast Health
- Yearly mammograms at age 40 and continuing for as long as a woman is in good health
- Clinical breast exam (CBE) every year for women aged 40 and over and every 3 years for women in their 20s and 30s
- Breast self-exam (BSE) for women starting in their 20s
- Screening mammograms are not recommended for average risk women under age 40
- Women with implants have screening mammograms at age 40 and continue as long as a woman is in good health
Women who are at high risk of breast cancer (due to a gene mutation, a strong family history, or previous radiation to the chest for cancer) should have a discussion with their health care provider, taking into account personal circumstances and preferences.
What is a Screening Mammogram?
Screening mammograms are x-ray exams of the breast that are used for women who have no breast symptoms or signs of breast cancer (such as previous abnormal mammogram). The goal of a screening mammogram is to find breast cancer when it is too small to be felt by a women or her doctor. A screening mammogram usually takes 2 views of each breast. Some women have breast tissue in the axillary (armpit) region and therefore may need to have more images so that the Radiologist is able to accurately assess the entire breast. OCWMG contracts with a Specialized Mammography Radiolgist who will interpret your mammogram within 24-48 hours to determine if there are any suspicious areas.
For every 1,000 women who have a screening mammogram:
- 100 patients are recalled to get more mammography or ultrasound
images, may times based on the type of tissue - 20 patients are recommended for a needle biopsy
- 5 patients are diagnosed with breast cancer
Whats New? 3D Tomosynthesis Mammography
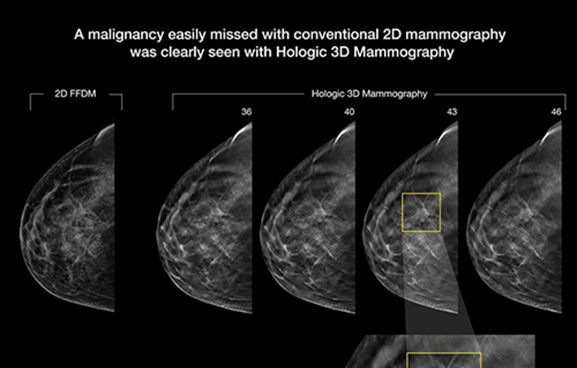
Conventional digital mammography produces one image of overlapping tissue, making it difficult to detect cancers. Performed with digital mammography using the same scanner, breast tomosynthesis takes multiple images of the entire breast. The X-ray tube moves in an arc around the breast while 11 images are taken during a 7-second examination. Then the information is sent to a computer, where it is assembled to produce clear, highly focused 3-dimensional images throughout the breast. It allows the radiologists to see through layers of tissue and examine areas of concern from all angles. Benefits can include:
- Earlier detection of small breast cancers that may be hidden during digital mammography
- Greater accuracy in pinpointing size, shape and location of abnormalities
- Fewer unnecessary biopsies or additional tests
- Greater likelihood of detecting multiple breast tumors, which occur in 15% of breast cancer patients
- Clearer images of dense breast tissue
-
Is there increased radiation with Tomosynthesis?
Tomosynthesis is safe. Radiation exporsure to the breast is very low. The radiation dose for a combined 2D/3D mammography exam is well below the acceptable limits defined by the FDA, and is only a fraction of the level of radiation everyone receives annually from the natural background of being outdoors. There is no evidence that this low level of radiation has any significant effect on the breasts. As with any x-ray, patients should inform their technologist before an exam if they are (or may be) pregnant.
-
When to schedule your mammogram
It is best to schedule your mammogram about a week after your menstrual period. Your breast won’t be as tender or swollen, which means less discomfort during the x-ray. OCWMG offers same day mammogram screening after your annual exam
-
What (and what not) to wear
Wear a 2-piece outfit because you will need to remove your top and bra. Do not apply deodorant, antiperspirant, powder, lotion, or ointment on or around your chest or armpit on the day of your mammogram. These products can appear as white spots on the x-ray and may necessitate unavoidable exposures.
-
Insurance
Under the Affordable Care Act, Medicare and almost all private insurance plans now cover yearly mammograms, with no-copay or out-of-pocket cost. The FDA has approved that 3D Tomosynthesis Mammography is acceptable for all breast tissue types and is no longer being used as “investigational” for most insurance companies. However, some insurances are only approving annual Conventional 2D Mammography. There is a possibility that the 3D portion may not be covered. If you receive a bill please go to our Resources page for billing information.
To schedule your mammogram, call (949) 829-5533 or contact us online.

